Today, ocular, and orbital ultrasound using B mode is an essential diagnostic aid technique for the ophthalmologist, previously it was reserved for specialists, but today it has become an excellent tool to help the general ophthalmologist. It is necessary that every ophthalmologist will be trained in this technique and takes advantage of its versatility, the possibility of being performed next to the patient and the few requirements that are needed to carry out the examination. But the most important thing of all is: to "lose the fear" of venturing to examine the patient.
 For this purpose, we want to give some tips, which allow you to handle the exam techniques to get the best and most useful results. First, you need to have a proper ultrasound device, we use the ABSolu® with the 15 MHz probes and the 20 MHz 5-ring, and the Compact Touch® with the 15MHz probe. The difference between them is that with 15MHz probe an initial "scan" can be performed with images focused on the posterior pole, while with the 20 MHz multifocal images are obtained from the vitreous to the retrobulbar orbit.
For this purpose, we want to give some tips, which allow you to handle the exam techniques to get the best and most useful results. First, you need to have a proper ultrasound device, we use the ABSolu® with the 15 MHz probes and the 20 MHz 5-ring, and the Compact Touch® with the 15MHz probe. The difference between them is that with 15MHz probe an initial "scan" can be performed with images focused on the posterior pole, while with the 20 MHz multifocal images are obtained from the vitreous to the retrobulbar orbit.
One must be convinced that the main task at the beginning is to determine if what you are seeing is "normal" or "pathological", although it seems incredible, the mere fact of being able to determine that what we are observing corresponds to either of these two categories, constitutes 50% of the task of the novice examiner. After one can do so, one must ascend to the next level: determining what is seen as pathological. Even at this moment it is not necessary to be an expert, since describing in detail what we are observing and its ultrasound characteristics: shape, size, reflectivity, brightness, vascularization or not, mobility, post movement etc. We can guide others about the nature of the injury. Later one can continue to improve and become an expert.
Tips and tricks for performing an exam
Once convinced of this we must observe the following recommendations to correctly perform the exam:
We must place the patient in a relaxed position, preferably semi-sitting, with the head in front of us and in front of the ultrasound screen, that way we can observe the position of the head, the direction of the gaze and correlate it with our examination. We must bear in mind that ultrasound is dynamic and both our hand holding the probe, and the patient's eye, must move. In this way we will make an adequate examination of both the posterior pole, and especially the periphery. A frequent mistake is to place the probe only pointing towards the posterior pole, without balancing it, or not asking the patient to move their eyes in different directions.
- The probes have a marker (usually a white line) that indicates the direction of the ultrasonic beam when leaving the piezoelectric crystal and defines the upper zone of the sectoral displacement of this. In simpler words, the line tells us what is superior in the image of the screen, in the case of the 20 MHz probe of 5 rings, this has a built-in motion sensor that after calibrating it to 12 hours, reflects on the screen the direction of the beam during the exam. Conventionally, the probe should always be placed pointing upwards or towards the patient's nose.
- Every exam begins with a circumferential sweep in a transverse way (oriented by the line) with 8 positions superior, supero-nasal, nasal, infero-nasal, inferior, infero-temporal, temporal and finally temporal superior. When examining each of these positions we must rotate our wrist so that the probe points to the most anterior region, then to the middle region and finally to the posterior area of the eyeball of each sweep zone.
- If we find any abnormality, we must combine this examination with the longitudinal approach, rotating the probe 90 degrees from the transverse position, since in this way we have the vision of the "examinated hour" clearly differentiating what is anterior and what is later in the ultrasound image. Having determined the time zone of the lesion and its middle or posterior anterior placement of the eyeball, we must proceed to "center" the image, that is, obtain a representation, where the lesion to be studied is located in the center of the screen, so we will obtain the maximum echo of it, at this time we can make the observation of the internal structure, its reflectivity, whether or not there are vascularizations, perform the measurements of it etc. We must not forget to vary the gain during the examination to better define the margins of the lesion, eliminate parasitic echoes and clearly define the ultrasound characteristics of the lesion.
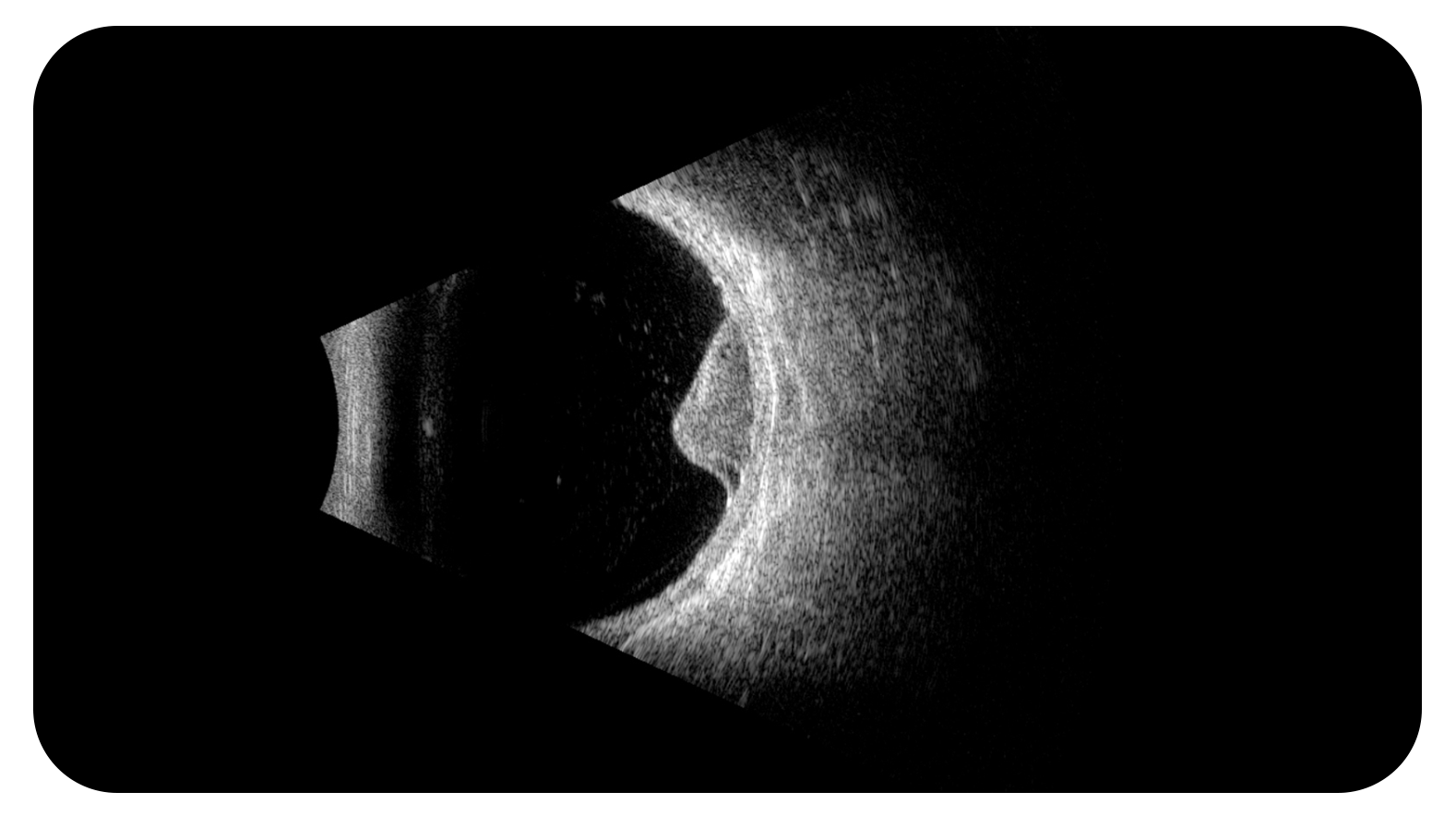
- It is important to be attentive to the ocular and orbital structures and when describing them to have an adequate order, it is preferable to make a reporting protocol, starting with the vitreous and its description, its mobility, adhesions: type of them: if they are strong or weak, their opacity, the presence of floaters, tractions and tears or vitreous detachment, in addition to other pathologies. Then go on to describe the retina in the posterior pole and in the periphery, its integrity, or if it is detached and also other lesions that can be observed. Once that is done, describe the choroid and the sclera, especially its thickness in the posterior pole as in the periphery or the presence of lesions that occupy space, then define it is find any lesion in the orbit, separating it from the extraocular muscles and the optic nerve which is what is normally seen more clearly.
Following these simple recommendations, we can feel that we can begin to properly master the exam with B mode in a progressive way gain experience in the exam, a final recommendation is always good to have someone who is your Mentor, to have a desire to continue learning despite making mistakes and if you can combine the ultrasound findings with other methods establish the comparisons that will serve us in the next exam.
Well then: wings and good wind.... Let's start mastering the exam with B mode without fear and with a lot of enthusiasm!