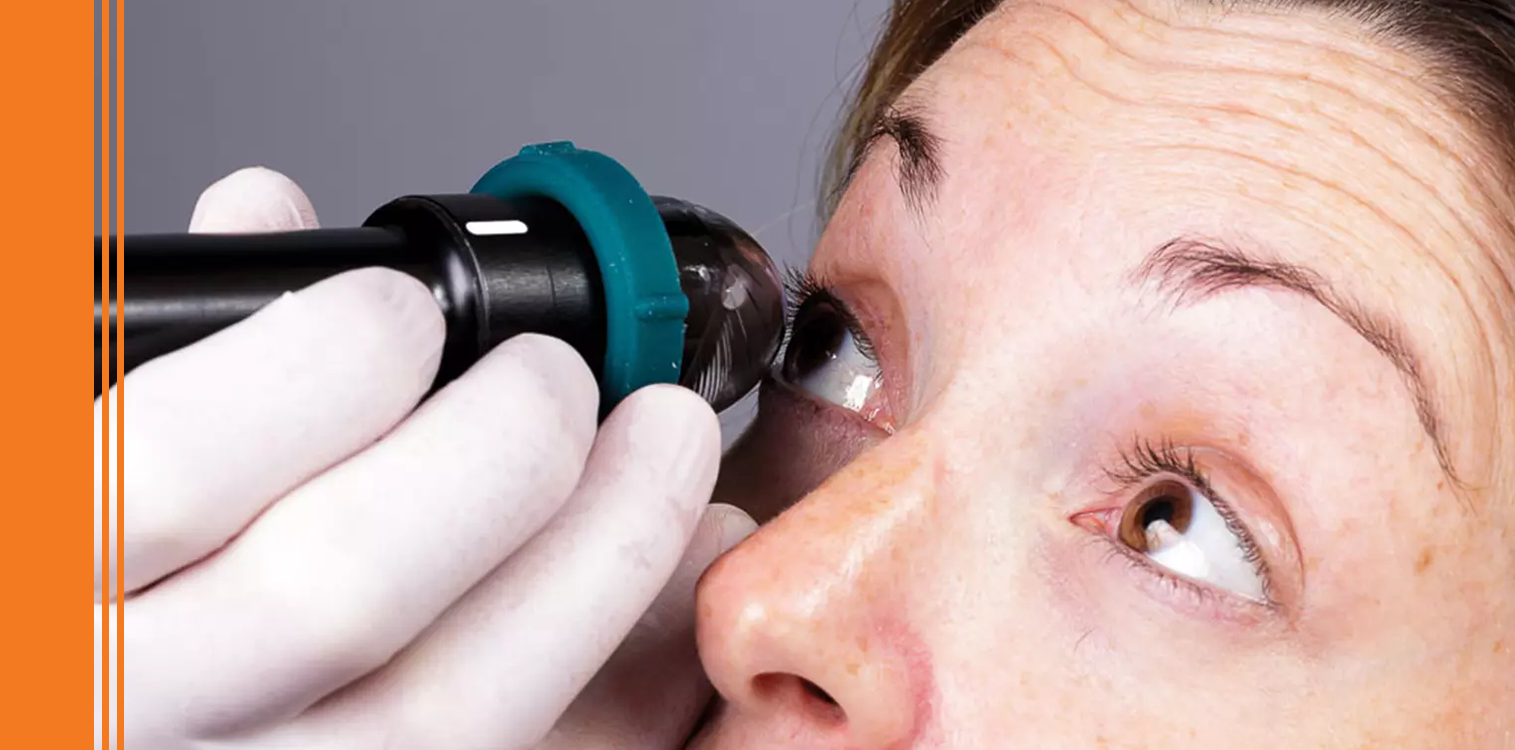
Ultrasonic biomicroscopy (UBM) is a valuable auxiliary method in the diagnosis of different pathologies of anterior segment. Unlike optical coherence tomography, UBM can display images of the deep structures of the anterior segment and the extreme periphery of retina. It has the advantage of being a dynamic examination, which usually does not need the collaboration of the patient, can be performed in the presence of opaque media and where fixation by the patient is not very important.
Nowadays the excellent resolution and penetration obtained by the new equipments with more powerful transducers allow us to have a new diagnostic aid tool available to everyone. In that sense we work with the new 50MHz probe, of the ABSolu® device, either using the ClearScan® or the immersion scleral shell.
However, the fact of being a "contact" exam causes many examiners to refrain from performing it, this is really surprising because anyone who performs eye exams is able to place, either a speculum between the eyelids or a three mirrors lens on the cornea.
Here's my first advice: Don't be afraid to perform a contact test, which is no more or less complicated than any other in ophthalmology.
Safety first!
The first thing we must keep in mind is that if the exam is carried out with the minimum safety conditions it is a simple, innocuous, fast procedure, with excellent results.
To perform a safe examination, we must be sure that patient is aware of the examination we are going to perform, my advice is: "an informed patient is a collaborating patient". Patient should come to the office without makeup from the skin of the eyelids or eyelashes, as well as contact lenses, if applicable. We must ensure that he/she do not suffer from any type of contact allergy especially to anesthetics, since topical drops of these medicament will be applied, to facilitate the examination
The next thing is to define if we use the ClearScan® or an immersion scleral shell because the transducer needs to be relatively far from the structures to be examined.
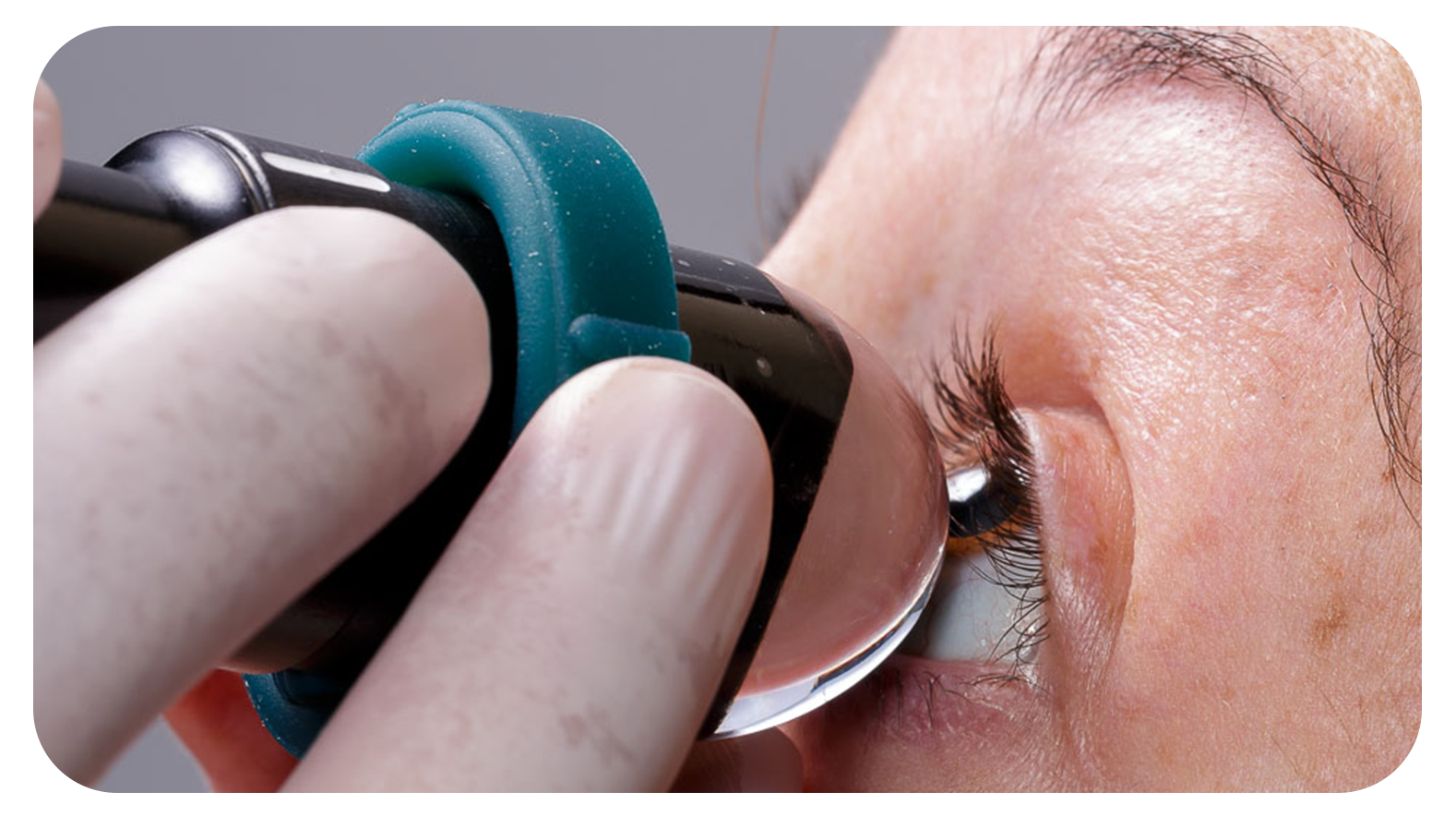
The ClearScan® is a disposable device that allows us to perform the examination on the patient in a sitting position, it must be filled with distilled water to avoid crystallization of the salts of the solutions such as BSS or sodium chloride on the piezoelectric crystal. The tension of the membrane of the ClearScan® must be regulated according to the sensitivity of the patient or the type of examination we wish to perform, must be very turgid in the examination of the cornea, eyelid lesions and superficial tumors and must have a relative elasticity when examining the angle and other retroiridian structures. We only have to maintain turgor if we want to make a pseudo indentation with the ClearScan®.
In the case of the immersion scleral shell, it is better to use a soft-edged silicone one, that has been previously disinfected with adequate solutions and that cleaned with plenty of water before performing the exam, thus avoiding irritation by substances outside the study. This scleral shell will be placed gently, on the conjunctiva surrounding the limbus, avoiding touching the cornea. Then it will be filled with water solution without minerals, avoiding stylized water that is harmful to the cornea.
Get to know your patient
An important tip is to establish the reason or why the study has been sent to us, to know what we are looking for with it. If it is our patient there is no problem, but usually colleagues send us patients to rule out a specific pathology and this must be clearly established in the medical order, before starting the examination, in this way we optimize the search for the pathology to search or corroborate it during the study.
Standardize your examinations
We always recommend an orderly, standardized examination, first doing a general 360 degrees “scanning”, with eye movements of the patient, according to the area we want to examine, and then concentrate on the area where we find any pathology.
An important tip for beginners is that: This examination is intended to discover if there is anything abnormal in the anterior and intermediate segment, so it is necessary to have previously examined "normal" eyes during training, before venturing to look for any pathology.
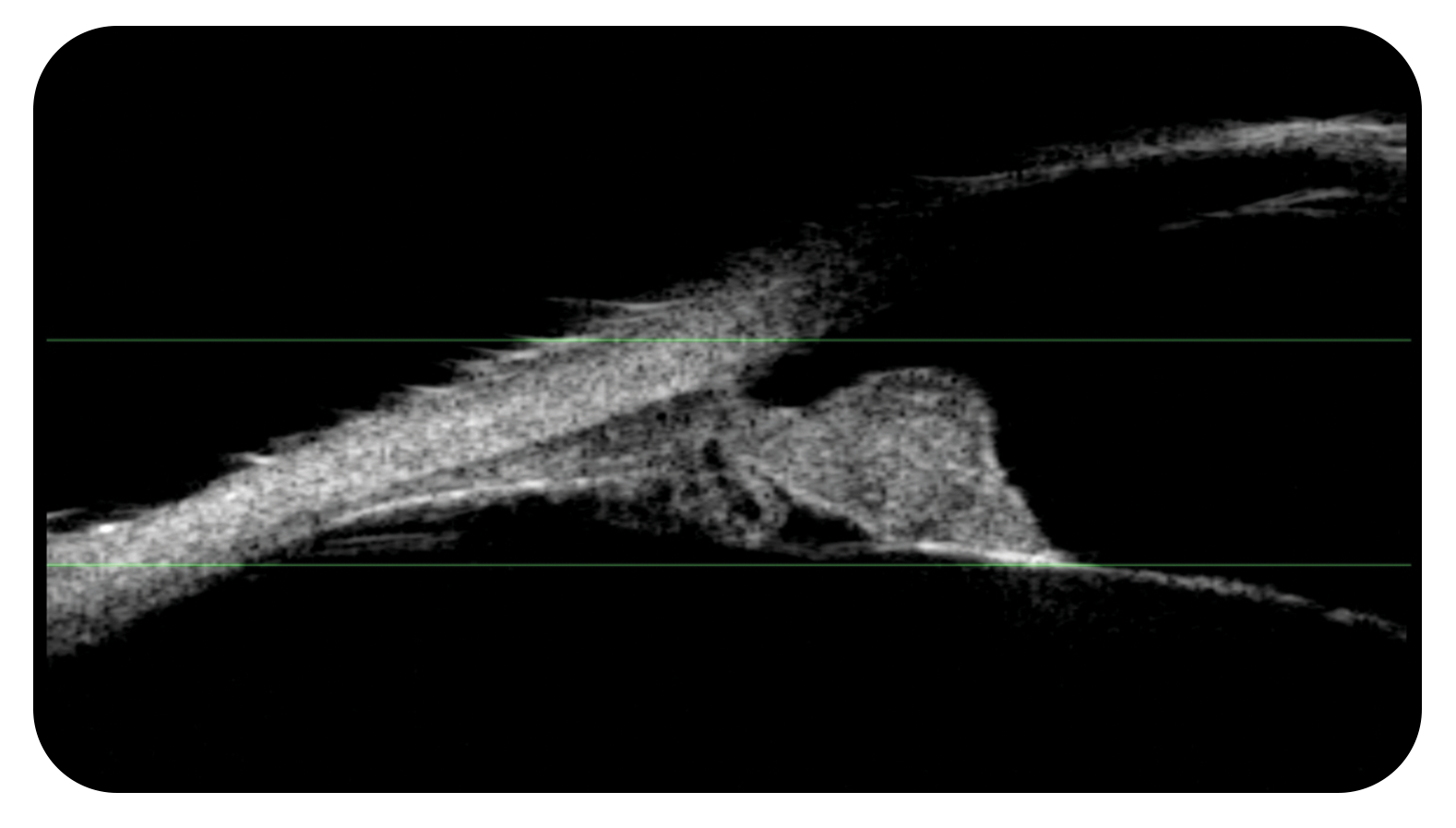
Just the fact of discovering an abnormality, whatever it may be, is important because generally this is 50% of the work to be done.
Then an important tip: Describe what is abnormal at sight, if you do not know the diagnosis at first it does not matter, whoever reads your description and has more experience can lead his diagnostic judgment. Then it is mandatory to reach the final diagnostic information, in order to establish a correlation between what you have observed and what was finally the pathology, this learning process should always be accompanied by a tutor or mentor to optimize learning.
In the training process it is absolutely necessary to compare our findings with other methods, sometimes even with pathology, in this way we will learn to correlate the lesions with their ultrasound image.
Following all these tips we must start without fear in learning this method, which will allow us to access areas where optical methods do not reach, in addition to being an operator-dependent exam will make us necessary in the diagnostic process driving us to improve every day and to study more enthusiastically the pathologies and other conditions that we will discover over time.
Our goal is to overcome the fear of performing the first exams over time and with a lot of patience we become experts in this fascinating diagnostic method.
My last advice, study the macroscopic pathology of the lesions to observe and correlate the clinic with your findings since you should never forget that this is a method of diagnostic aid and that combined with the clinic will give you a considerable advantage with those colleagues who do not dare to perform this examination.